Retinal Detachment & Retinal Tears
The retina is a thin layer of tissue at the back of the eye that processes light and sends signals to your brain, allowing you to see clearly. When the retina develops a tear or becomes detached from its supporting layers, vision is put at serious risk. These are true eye emergencies — without immediate treatment, permanent blindness may occur.
Fortunately, with today’s advanced diagnostic tools and surgical techniques, retinal tears and detachments can often be treated successfully if caught early.
What Is a Retinal Tear?
A retinal tear occurs when the vitreous gel inside the eye pulls too strongly on the retina, causing a small break. These tears create an opening where fluid can pass underneath the retina.
If untreated, a tear may progress to a retinal detachment.
Retinal tears are more common in people with age-related vitreous changes, high levels of nearsightedness, or a history of eye trauma. While tears may not always cause symptoms, many patients report seeing flashes of light or new floaters when they first occur.
What Is Retinal Detachment?
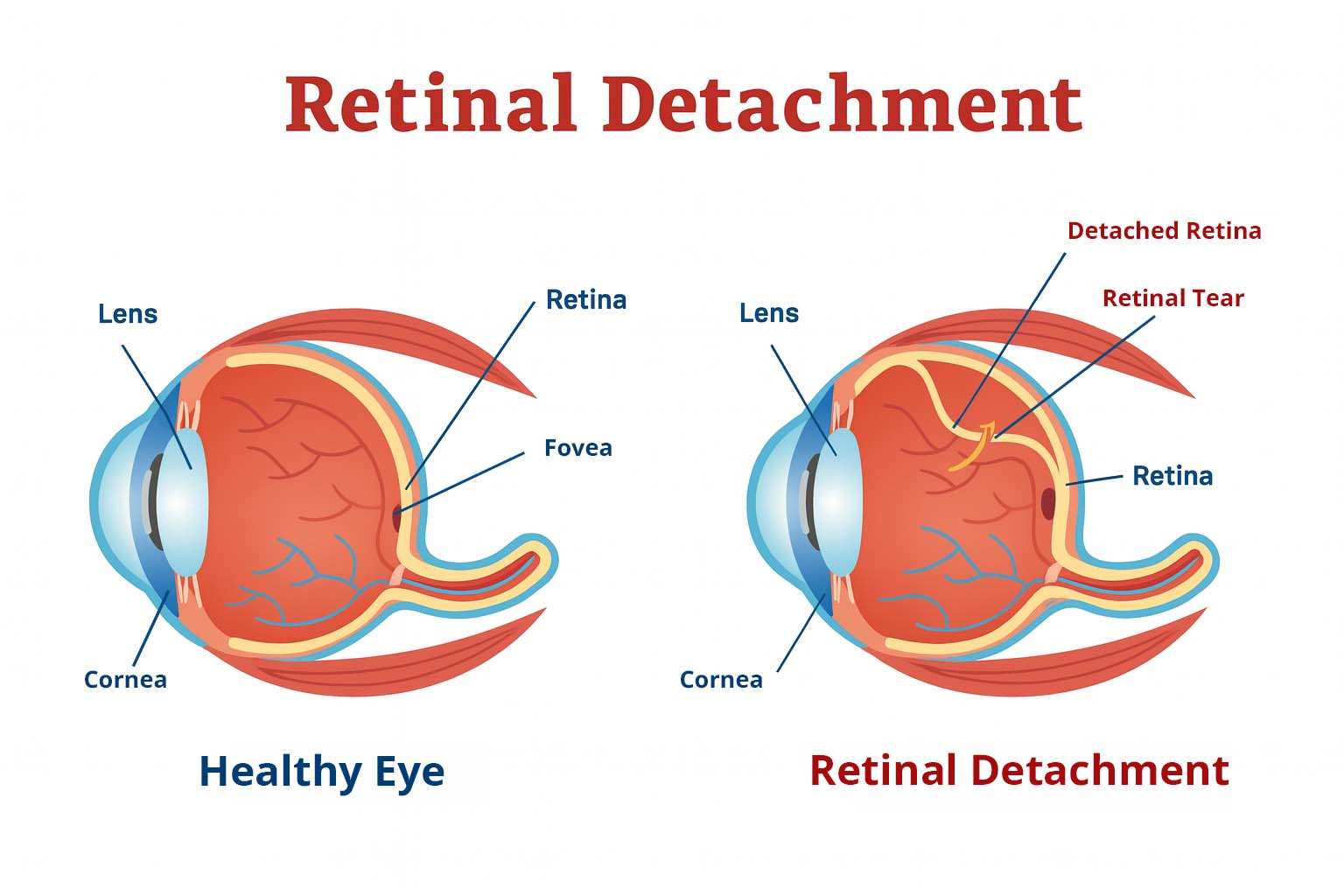
Retinal detachment happens when the retina separates from the tissue beneath it. This separation cuts off the retina’s blood supply and prevents it from functioning properly. Vision loss from a retinal detachment can be severe and permanent if not treated quickly.
Unlike many eye conditions, retinal detachment is painless, which is why recognizing the warning signs is so important. Early treatment offers the best chance to restore vision.
Read More About a Detached Retina [PDF]Types of Retinal Detachment
Rhegmatogenous Retinal Detachment
The most common type, caused by a retinal tear. Fluid passes through the tear and accumulates under the retina, lifting it away from the back of the eye.
Tractional Retinal Detachment
Scar tissue on the retinal surface pulls the retina away. This type is more common in people with advanced diabetic eye disease or other vascular conditions.
Exudative Retinal Detachment
Fluid builds up beneath the retina without a tear or hole. Causes include inflammation, tumors, or uncontrolled hypertension.
Symptoms to Watch For
Retinal tears and detachments often start suddenly. Contact your eye doctor or retina specialist immediately if you notice:
- A sudden increase in floaters (tiny black specks or cobweb-like spots)
- Flashes of light in your side (peripheral) vision
- Blurred or distorted vision
- A curtain-like shadow moving across your vision
- Sudden, painless loss of vision in one eye
These symptoms should never be ignored. Immediate evaluation can save your sight.
 Example of floaters in your vision
Example of floaters in your vision
Causes and Risk Factors
Retinal tears and detachments can affect anyone, but certain factors increase the risk:
- Aging, which causes the vitreous gel to shrink and pull away from the retina
- High myopia (severe nearsightedness)
- Family history of retinal detachment
- Previous eye surgery, such as cataract removal
- Significant eye trauma or injury
- Diabetes and associated retinal vascular disease
Understanding these risks helps patients take preventive steps, like regular dilated eye exams and prompt attention to new symptoms.
How Is It Diagnosed?
A retina specialist will perform a comprehensive dilated eye exam to carefully examine the retina. Additional tests may include:
- Optical Coherence Tomography (OCT): Provides high-resolution images of the retina’s layers, showing detachments and swelling.
- Ocular Ultrasound: Used when bleeding blocks the view of the retina.
- Fundus Photography: Documents the condition and helps track changes over time.
Because retinal detachments progress quickly, diagnosis and treatment often occur the same day symptoms appear.
Treatment Options
Treatment depends on whether the retina is torn or fully detached, and on the type and extent of the damage.
Laser Photocoagulation / Cryopexy (for Tears)
For small retinal tears, a laser or freezing probe creates a scar that seals the retina to the underlying tissue. This prevents fluid from passing through and causing a detachment.
Pneumatic Retinopexy
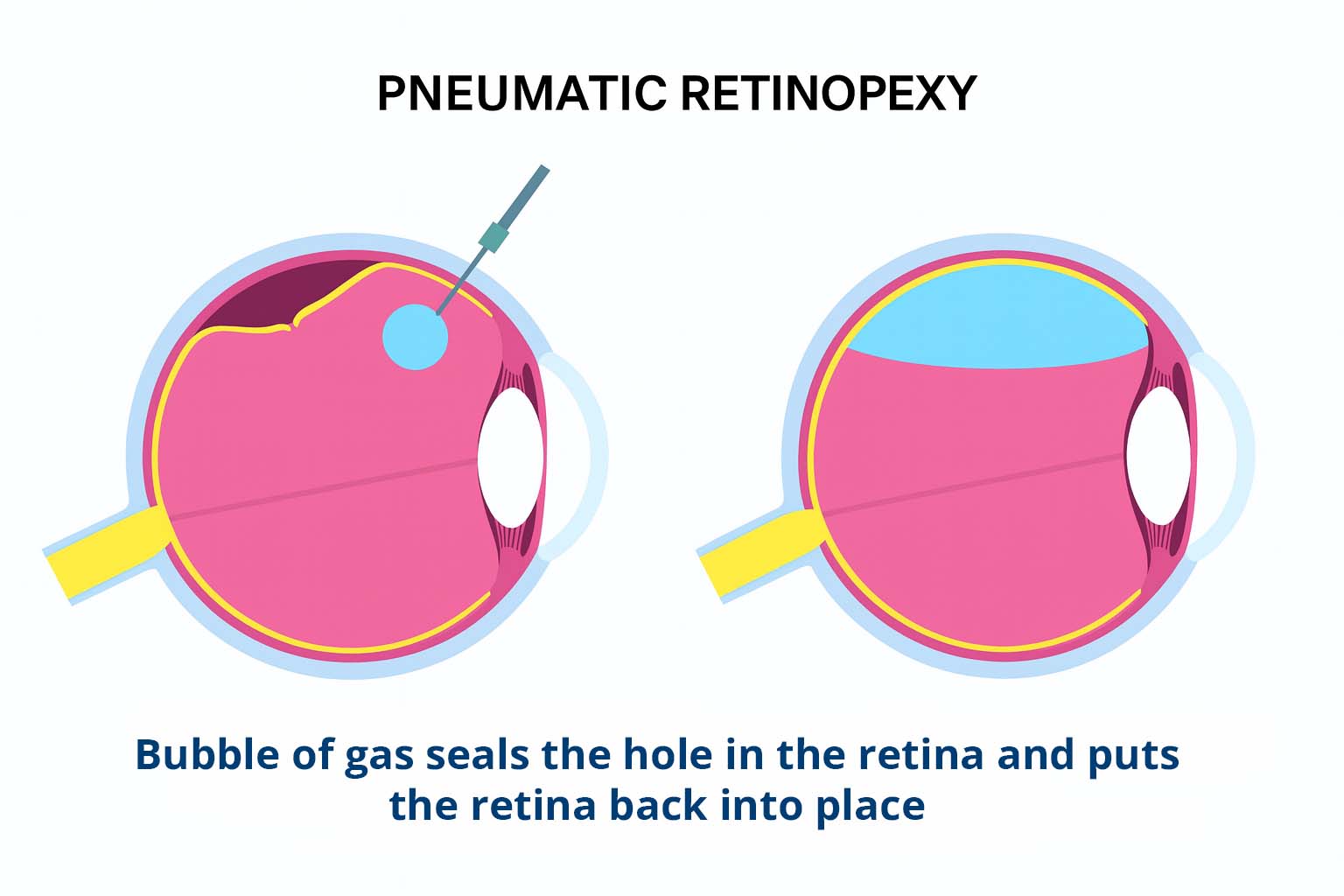
A small gas bubble is injected into the eye to press the retina back into place. This is often combined with laser or cryopexy to permanently seal the tear. Patients may need to keep their head in a specific position for several days to allow the bubble to work.
Scleral Buckle Surgery
A silicone band is placed around the eye to gently push the outer wall against the retina, closing tears and supporting reattachment. This technique is effective for more complex detachments.
Vitrectomy
In this surgery, the vitreous gel is removed and replaced with a gas bubble or silicone oil, which pushes the retina back into position. The bubble eventually dissolves or is removed in a follow-up procedure.
Recovery & Prognosis
- Success rates are high: Over 90% of detachments can be reattached with one or more surgeries.
- Vision recovery depends on timing: If the central retina (macula) remains attached, vision is more likely to be preserved.
- Recovery requirements: Some patients must maintain strict face-down positioning after surgery to keep a bubble in place.
- Follow-up care: Regular visits are essential to monitor healing and prevent recurrence.
Frequently Asked Questions
-
What is the difference between a retinal tear and a retinal detachment?
A retinal tear is a small break in the retina, often caused when the vitreous gel inside the eye pulls too hard on the retina. While a tear alone may not cause vision loss, it creates an opening where fluid can leak underneath the retina. If this happens, the retina can begin to separate from the back of the eye, leading to a retinal detachment. Retinal detachment is much more serious because the retina is no longer receiving oxygen and nutrients, and vision can be permanently damaged. The main difference is that a tear is an early stage that can be treated quickly with laser or cryotherapy, while a detachment is a more advanced condition requiring urgent surgery.
-
What symptoms should I watch for with retinal detachment?
Retinal detachments usually start with warning signs. The most common are new floaters (tiny spots, lines, or cobweb shapes that move in your vision) or sudden flashes of light in your side vision. Some patients notice blurred or distorted vision, or they describe a “curtain” or shadow moving across their sight. In advanced cases, there may be sudden, painless loss of vision in one eye. These symptoms require immediate attention — a retinal detachment will not get better on its own, and delaying care makes vision loss more likely. If you experience these warning signs, call your eye doctor or retina specialist right away.
-
Is retinal detachment an emergency?
Yes. Retinal detachment is considered a true eye emergency. Without treatment, the retina cannot function properly and vision loss can become permanent. In fact, once the central part of the retina (the macula) detaches, the chances of fully restoring vision drop significantly. The good news is that modern treatments, including laser therapy and surgery, are highly successful when performed promptly. If you notice sudden flashes, floaters, or a curtain-like shadow in your vision, seek care immediately. Even if symptoms seem to come and go, it’s best to treat them as urgent. Acting quickly could save your sight.
-
Can a retinal tear heal on its own?
No. A retinal tear will not heal on its own. In some cases, a small tear may not cause immediate symptoms, but the risk is that fluid will pass through the opening and lead to a retinal detachment. To prevent this, retinal tears are typically treated with either laser photocoagulation or cryopexy (a freezing treatment). Both methods create a scar that seals the retina to the back of the eye, closing off the tear and preventing progression. These treatments are usually performed in-office and are quick, safe, and effective. Prompt treatment of a tear can prevent the need for more complex surgery later.
-
What are the treatment options for retinal detachment?
The treatment for retinal detachment depends on the severity and type. Small tears may be treated with laser or freezing therapy, but a full detachment usually requires surgery. Common surgical options include:
- Pneumatic retinopexy: A gas bubble is placed in the eye to press the retina back in place.
- Scleral buckle: A silicone band is placed around the eye to support the retina.
- Vitrectomy: The vitreous gel is removed and replaced with gas or silicone oil to reattach the retina.
Each procedure has specific uses, and your retina specialist will choose the best approach. With prompt surgery, more than 90% of detachments can be successfully repaired.
-
How long is recovery after retinal detachment surgery?
Recovery after surgery can vary depending on the procedure performed and the severity of the detachment. In many cases, patients need to rest for at least 1–2 weeks, with restrictions on heavy lifting and strenuous activity. If a gas bubble is placed in the eye, patients may need to keep their head in a specific position, sometimes face-down, for several days to allow the bubble to press on the retina. Vision improvement is usually gradual and may continue for several months. Follow-up visits are important to make sure the retina is healing properly. While some vision loss may be permanent, many patients regain useful sight and can return to normal daily activities with time.
-
What are the chances of regaining vision after surgery?
The outlook after retinal detachment surgery depends on several factors, especially whether the macula (the central retina responsible for sharp vision) was still attached at the time of surgery. If the macula remains intact, many patients recover good vision. If the macula has detached, the outcome is less predictable, and vision may not fully return to normal. Success also depends on how quickly treatment is performed. In general, over 90% of retinal detachments can be reattached with surgery, and many patients regain useful vision for reading, driving, and daily life. The most important step is seeking immediate care when symptoms begin.
When to See a Retina Specialist
Retinal tears and detachments are true emergencies. If you notice sudden floaters, flashes, or a curtain across your vision, call your eye doctor or retina specialist immediately.
Even without symptoms, patients with risk factors should schedule annual dilated eye exams. Early detection and treatment offer the best chance of saving your sight.

Don’t Wait — Protect Your Vision Now
Retinal tears and detachments are true eye emergencies. If you notice sudden floaters, flashes of light, or a curtain in your vision, seek help immediately. Early treatment can save your sight.
Request an Appointment or call 208-535-4900 for immediate care at Teton Retinal Institute.
